Medical journal releases infographic and consultation tips for identifying pelvic girdle pain affecting up to one in five pregnant women.
Sarah Mitchell winced as she climbed the stairs to her Canterbury flat, her hand pressed against her lower back. At 20 weeks pregnant with her second child, the sharp pain radiating through her hips and groin had begun disrupting her sleep and making simple tasks feel impossible. What Sarah didn’t know was that she was experiencing one of pregnancy’s most common yet under-recognised conditions.
The Hidden Pregnancy Challenge
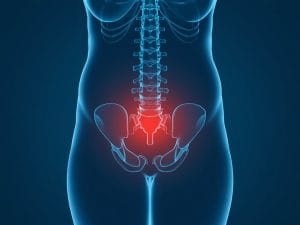
Pregnancy-related pelvic girdle pain affects up to one in five expectant mothers across the UK, according to some studies. Yet many women struggle to get proper diagnosis and treatment for this debilitating condition that causes pain in the lower back, buttocks, hips, pubic bone, groins or inner thighs.
The pain typically emerges around week 18 of pregnancy. But diagnosis remains tricky – current methods rely on pain provocation tests that have poor reliability when using bony landmarks or checking for asymmetry, according to clinical research.
Women with previous back pain, prior pelvic girdle pain, or higher BMI at the start of pregnancy face increased risk. The condition can severely impact daily activities, from walking upstairs to getting dressed.
Early Action Makes All the Difference
The Royal College of Obstetricians and Gynaecologists emphasises that early identification and management can control symptoms and prevent chronic pain developing. Simple changes make a real difference.
Practical recommendations include wearing low-heeled shoes, reducing weight-bearing activities, and avoiding movements that spread the hips apart. Taking smaller steps when walking and avoiding positions that trigger pain can provide immediate relief.
Management focuses on conservative approaches – physiotherapy, pelvic support belts, and pacing daily activities. Research shows that about 10% of affected women report long-term issues lasting up to 11 years after birth, making prompt treatment essential.
But there’s good news. The condition causes no structural damage, and individualised care can steeply improve outcomes through pregnancy and beyond.
Supporting Better Care
The BMJ’s new educational resources aim to help clinicians recognise and manage pelvic girdle pain more effectively. The infographic provides clear guidance on history-taking, examination techniques, and self-management strategies that doctors can share with patients.
This matters because many women don’t report their symptoms, assuming pain is just a normal part of pregnancy. Others receive delayed diagnosis, leading to reduced quality of life and family disruption that could have been prevented.
Source: @bmj_latest
Key Takeaways
- Pregnancy-related pelvic girdle pain affects around 20% of pregnant women, typically starting at week 18
- Early physiotherapy and lifestyle modifications can prevent chronic pain and disability
- Simple changes like wearing low heels and taking smaller steps provide immediate symptom relief
What This Means for Kent Residents
Kent pregnant women experiencing pelvic or back pain should contact their GP or maternity team early rather than assuming discomfort is inevitable. Local NHS services through NHS Kent and Medway ICB offer pelvic girdle pain assessment, while hospitals including Medway Maritime and Kent and Canterbury provide specialist women’s health physiotherapy through their antenatal clinics. For urgent concerns, residents can call NHS 111 for advice, or attend A&E if pain becomes severe – but early intervention through routine maternity care offers the best chance of managing symptoms effectively throughout pregnancy and preventing long-term complications.